
Choose Your Language:
Posted by: The Sumaira Foundation in NMOSD, Patient, Voices of NMO
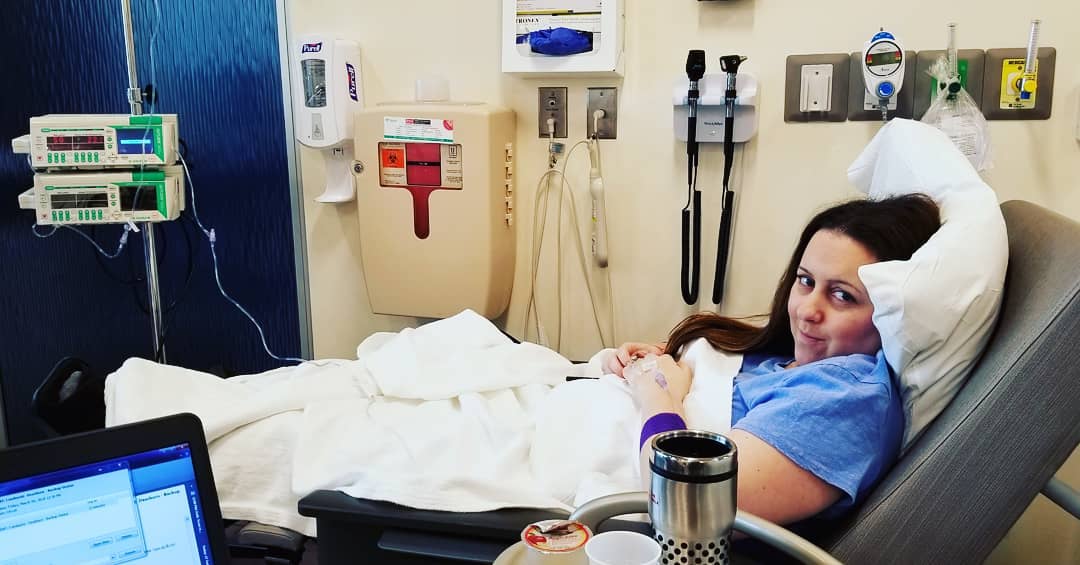
Jamie was diagnosed with Non-Hodgkins Lymphoma at the age of 35. Her condition was such that she didn’t need treatment, just monitoring. She was even healthy enough to have a second child. After the birth, though, she was put on Rituximab for the lymphoma, once a week for four weeks.
Two years later, one night in September of 2017, Jamie felt a dramatic pop under her ribs on the left side. Soon afterwards, she noticed she was experiencing neck pain, and then frequent nausea and hiccups. The hiccups went on for hours at a time and often made Jamie throw up. She realized over time that she could stop the hiccups by vomiting, so at times she did so deliberately. These symptoms led Jamie to the hospital three times, where they diagnosed gastritis and sent her home. She followed up with a gastroenterology specialist who did an endoscopy, which showed nothing amiss.
In December, on her way home from work one day, Jamie noticed that she was dragging her left leg. Over the next few days, the leg got worse and worse, until she was completely paralyzed. It was then that she had the first of many MRIs. This scan showed multiple lesions, and a neurologist recommended Jamie go straight to the emergency room. But since she had a trusted oncologist, she called him instead, and he direct admitted her to the hospital, where Jamie stayed for three weeks.
She was tested, poked and prodded, while being given five days of Solumedrol (IV steroids), five days of plasmapheresis and then five days of IVIG (intravenous immunoglobulin). Jamie remembers being able to wiggle her toes on the third day of plasmapheresis, and she improved slowly during her days in the hospital, in-patient rehab and then out-patient rehab.
The fear was that her cancer had turned into a more virulent form of lymphoma. One of the doctors in the New Jersey hospital where Jamie was being treated recommended she go to Memorial Sloan Kettering in New York for a second opinion. It was there that Jamie was told she had NMO, not Intervascular Lymphoma.
Jamie’s cousins, some of whom are doctors, sent her immediately to see Dr. Michael Levy at Johns Hopkins, who explained her new condition, what to expect, and recommended treatments. Given the cancer though, Jamie started back on Rituximab, but at a level for cancer – once a week for four weeks. This was in March. The next treatment was to have been in September.
Instead, in July, while planning a 40th birthday party for her husband, mourning the loss of her grandmother and celebrating the birth of her nephew, Jamie drove her daughter to camp, and went in to sign some papers. She couldn’t make her hand work. The feeling fluctuated between numbness, tingling and burning. Her oncologist admitted Jamie to the hospital again the next day, where she was given the five-day Solumedrol regimen and plasmapheresis over a two-week stay.

Jamie can walk and run after her children, now three and six. When they are home, Jamie is sure to be up and active, despite regular pain, which has gotten worse over time, especially after her second relapse.
When Jamie was diagnosed with cancer, she thought it would wreak havoc on her life. But no – NMO – this rare and unknown disorder – has caused far more damage.
At only 38, Jamie is too young for these dual burdens. But despite her diagnoses, ongoing treatments and crippling pain, Jamie is committed to being the best daughter, sister, wife and mother she can be.
Sometimes, when holding hands with her kids, a child might let go without Jamie feeling it. On the other hand, sometimes they tell her she is holding too tight. Given her love for her family, though, and given her condition, we might all agree that it just may never be too tight.
As told to Gabriela Romanow in October 2018