
Choose Your Language:
Posted by: The Sumaira Foundation in NMOSD, Patient, Voices of NMO
And then imagine, that, thank goodness, your husband is in the car with you and takes over driving before you get into an accident. You assume something crazy happened and so you continue heading to work, where, you think,

This happened to Theresa. She was 23 years old. In an hour, her hands still didn’t work, and she experienced both burning and numbness extending from those paralyzed hands up through her arms, to her chest and across her back, then down her legs and to her feet. She became so weak that she couldn’t even direct her fingers to type on the touchscreen of her phone.
Theresa went to the ER and said she had neurological symptoms she couldn’t explain. They had started the night before, with some strange sensations in both arms that had felt like muscle spasms. They went away, and she didn’t think anything of it. That night, she explained, she had the nightmare car ride and the worsening of her symptoms over the next hours. The ER doctor suggested she had had a panic attack and gave her Ativan. But when her body didn’t respond to that medication, he admitted Theresa into the hospital.
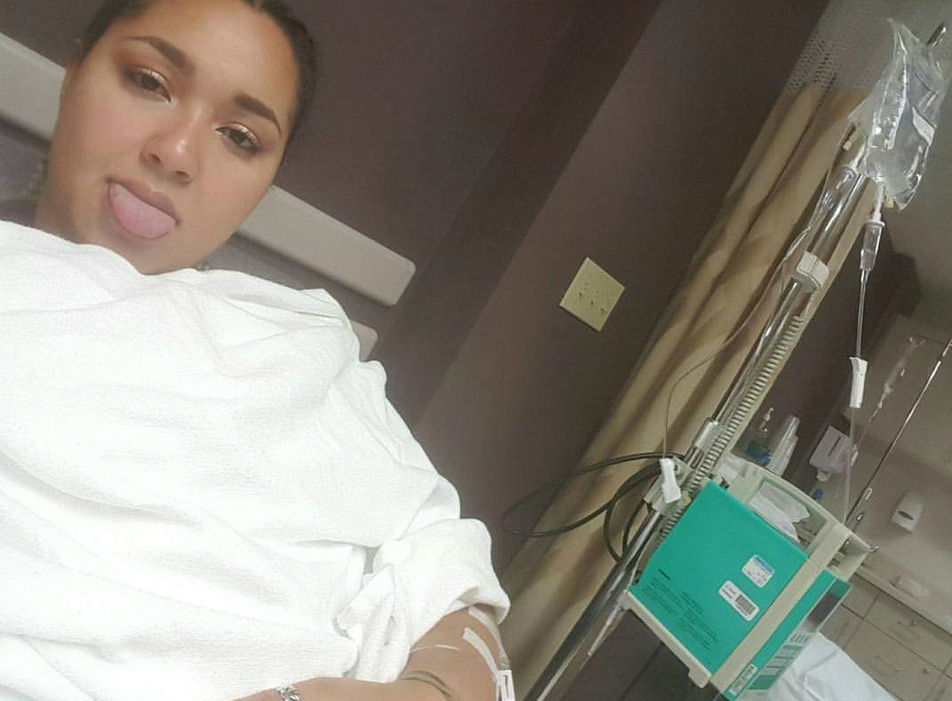
The next morning, Theresa couldn’t feel the lumbar puncture that was administered (one good thing about her numbness!) She then had a regular MRI, which showed enough to call for a contrast MRI. With that test, the doctors saw a lesion extending from C4 – T2 in her spinal cord. Four days after being admitted, Theresa was told she had idiopathic transverse myelitis. They said it was a rare condition, and that, once her symptoms resolved, it wouldn’t happen again and she’d be completely fine. Not until her 6th day in the hospital, did she get intravenous steroids. She had a five-day course of Solumedrol – two days in hospital and three at home.
For the next eight months, visiting physical and occupational therapists worked with Theresa at her home. It took all that time before she was able to sign her name properly or to walk with a cane. In some ways she was improving; in others, her deficits were worsening. She was sent to a new neurologist who saw that Theresa had had a second lesion at some time during those months, and so he tested her for a raft of neurological disorders. He told her that, among the possible diagnoses he postulated, NMO would be the worst. Of course, Theresa was indeed diagnosed with sero-negative (for both AQP4 and MOG) NMOSD. Theresa began researching NMO on her own, and took herself to another doctor for a second opinion, where her diagnosis was confirmed.
Theresa was put on Rituximab which has worked for her. Still, her residual symptoms from the extensive nerve damage she had suffered were terrible and widespread, including but not limited to tremors, spasms, abdominal banding, migraines, insomnia, nausea, vertigo, a neurogenic bladder and “heavy leg syndrome” in which gravity seems to make her legs feel very heavy after walking even very short distances.
 Theresa had been a personal care assistant for patients with special needs, including those with Downs Syndrome and Cerebral Palsy. There was no way she could return to that very physical and emotional work, as her own body had fallen apart. She used up all her medical leave and ended up on long-term disability. At first, she was paid 60% of her salary through the insurance company Unum, which Theresa reports offered kind and responsible support. They helped find her a lawyer who applied for disability benefits from social security for Theresa at age 23. Like many other applicants, Theresa has been declined for these benefits multiple times. Now working on this on her own, she is persisting.
Theresa had been a personal care assistant for patients with special needs, including those with Downs Syndrome and Cerebral Palsy. There was no way she could return to that very physical and emotional work, as her own body had fallen apart. She used up all her medical leave and ended up on long-term disability. At first, she was paid 60% of her salary through the insurance company Unum, which Theresa reports offered kind and responsible support. They helped find her a lawyer who applied for disability benefits from social security for Theresa at age 23. Like many other applicants, Theresa has been declined for these benefits multiple times. Now working on this on her own, she is persisting.
Theresa, a young woman, married only three years, and at the time excommunicated from much of her family, felt alone with her husband fighting a baffling monstrous disease they had never heard of that would never go away, thinking she was the only NMO patient on the east coast. She fell into a cycle of anxiety attacks and deep depression.
Over time, and with professional care, Theresa emerged from the depths and worked on mending bonds with her family. She found some NMO sites on Facebook, and was thrilled when she heard about the New England NMO Patient Day in Boston, where she learned more about NMO and met other local patients. She continues to do physical and occupational therapy, and has found that aquatherapy is the most powerful treatment – she is able to do much more in the water than she can on land, and she doesn’t hurt as much afterwards.
Theresa has learned to take life a day at a time. She sees other disease sufferers harbor major goals, and watches repeated disappointments. Instead, what works for this strong young woman is to develop small goals that can uplift her with each little step. She recommends being honest with yourself and others. It took Theresa some time to accept, for example, that she was no longer independent – something she had only recently attained as a young adult. Her regret over this loss was deep and sincere. And yet she is able to hold on to the fact that she has her husband’s loving support; her family and friends are now there for her; and she works with a network of skilled physicians and their entire teams who care very well for her. Theresa knows things could be worse – she saw many of those situations in her professional life. For this, Theresa is grateful. She acknowledges the cards that she has been dealt, faces them with strength; and each day, rises to take control of her life.
As told by Gabriela Romanow in October 2019