
Choose Your Language:
Posted by: The Sumaira Foundation in MOGAD, Patient, Voices of NMO

In 2012 I completed my master’s degree, which allowed me to change careers. I was leaving behind the demands of being a first responder. I enjoyed being a paramedic and loved working in law enforcement, but the truth was it had taken a toll on me. I was looking forward to a respite from the chaos and excited about a sustainable future.
I advanced quickly in my new field. By 2015, I was settling into my new position when I was promoted to an acting member of senior leadership.
It had been an awful winter, and I was battling a cold. A few weeks had gone by, and I couldn’t shake the cold. On April 8th, after dinner with a friend, my family took me to a local outpatient urgent care. I had bronchitis and pneumonia; they gave me some antibiotics and sent me on my way.
My symptoms got worse. I developed a crushing headache which I attributed to constant coughing and what felt like my brain rattling around. Late that evening, my left eye was getting blurry, and this was the first time I got a little worried. I figured it was because I was tired from not sleeping well.
On April 13th, I was taken to the ER by my wife. The doctor said there was sinus pressure causing the eye problem. They changed my medications and sent me home.
The next few days, I continued to feel worse. At about 0330 hours on April 15, I woke up and could barely stand; between the weakness in my legs and severe abdominal pain, I just could not do it. I asked my wife to take me back to the ER.
My wife got me to the hospital around 5 a.m. There was a flurry of tests, residents, therapists, attendings, and lord only knows who else. Nobody was sure what was going on.
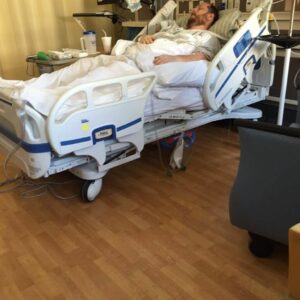
The doctors decided to admit me but could not decide who should do it. So here I am, lying paralyzed in bed. My wife is sitting beside me, watching this downward spiral. Our 13-year-old son is at home by himself, our family is four hours away, and the doctors are arguing over who should take the case. Thankfully the ER staff pointed that they didn’t care who did it, but it needed to happen quickly.
I was admitted to an ICU until the doctors were comfortable that my symptoms were not progressing. I was moved to a step-down unit while they tried to piece it all together.
I was fortunate enough to have a string of nurses and aides who would be critical to my future. First, there was Jen. She came into my room to check on me when my wife stepped out. I dealt with everything well, but my doubts and fears were loudest when alone. In these moments when I did not have to be strong for others, I would find myself starting to crumble.
Jen saw me trying to regain my composure. She stopped what she was doing, came over, took my hand in hers, and just held it tight. Once I was able to take a deep breath, she gently let it go and returned to her tasks. Before leaving, she let me know if I needed anything to let her know. Her eye contact spoke volumes to me. There was no judgment; there was no pep talk, no “I understand.” It was simply “I can see you. I can hear you. I am here for you,” and it was powerful.
Then there was the other Jen; she was tough and relentless. She questioned why more extensive imaging was not done. A few phone calls later, and I was off to radiology. The scans revealed a massive lesion starting at T3 encompassing my entire thoracic spine. I was moved to ICU shortly after that and started on high-dose steroids.
I had a string of terrible experiences with some members of my care team that left me humiliated and degraded.
Incident #1: The first experience was with the “skin inspection team.” Two women came in one morning to check for skin breakdowns. They introduced themselves and explained what they needed to do. They rolled onto my left side, my gown is completely open as they check me. I hear the room door slide open behind me, the curtain gets pulled back, and a third woman starts talking to the two that rolled me on my side. From the conversation, this new person was a part of their team, I also realize she had the door and curtain wide open to the hallway and everyone walking by. At that moment, if I had the ability to use my legs to do anything in the world, I probably would have chosen to crawl under my bed and hide. I wish I could say I was humiliated but I was dehumanized. Helpless, I just laid there and cried.
Incident #2: After a few days of high-dose steroids, I regained some gross motor function of my legs and occupational therapy was ordered. After numerous delays, cancellations, and no-shows, two therapists showed up. They told me how busy things were and how they were trying to get to me but there was so much to do.
If you want to isolate a person and minimize their self-worth, tell them how you are too busy for them and that everything else you have to do is a higher priority. I do not doubt they were busy, but this is not how you develop rapport, this is not how you develop trust, this is not how you treat people.
They began the evaluation, between the questions they were asking me, I got to listen to the details of their conversation that covered every aspect of their personal life. I was able to appreciate the nature of their relationship but was clearly the third wheel in this situation. I began to wonder if I even needed to be there. I felt ignored but brushed it off as being overly sensitive. They asked if I could stand, and I said “no”, but they wanted to try anyway. I was nervous.
I am a big guy and was worried that the therapists were obviously strong and knew how to move people, but I was dead weight. I suggested that they get an extra set of hands. They brushed me off my repeated requests and proceeded to get me sitting on the edge of the bed, one on each side, and hoisted me up and face-first into the recliner chair that was fortunate enough to break my fall. Helpless, I just laid there and cried.
Thankfully, I was buoyed by the nurses and nurses’ aides who were kind and their compassion extended beyond me and to my wife, who was struggling in her own right. One nurse, in particular, would be critical to me. She worked hard to make me smile, and she worked to make me see that those small, barely perceivable incremental changes, were progress. She cared for my broken body, but she was equally concerned about me as a person. Lori, came into my room to check my lines and see if I needed anything. She could see that I was struggling and just spent a few minutes checking things over and over. In retrospect, I realize it was a stall tactic to keep me talking. We talked about overcoming struggles and faith. She shared her own story of tragedy and loss and having to overcome. It is her story so I will not elaborate but to say the strength and courage she exhibited, the ability to keep pushing is tremendous. We both shed a few tears that night as she held my hand. I owe her so much.
A few days later, I was lying in bed when the neurology resident came in for his morning check-in. He was leaning against the red flip-top biohazard container on the wall opposite of my bed, arms crossed; he confidently declared, “We know what is going on.”

He went on to explain, “the same as MS, but you won’t get brain lesions,” my immune system was attacking my spine and optic nerve. I was stunned and had so many questions:
So what does this mean moving forward?
What is the prognosis?
Can I still work?
How can I drive a car?
Would I walk again?
Will I be permanently blind?
All the questions I needed answers to came to a halt as he spoke with a cocky smile. He told me, and as you can imagine, these words are seared into my brain, “You will go blind a little here and there, and in about five years, you will be blind. After that, it is a matter of time until you get a lesion high enough on the spine to knock out your respiratory drive. If you are lucky enough to get the treatment, you will be on a vent…many people die of pneumonia at that point.”
I remember my entire world became so small. Nothing existed beyond the doctor’s voice, those words, and that self-aggrandizing smile. I was trying to gather my thoughts and shake off the blow I just took. He spoke again, “I will be back for morning rounds.” He turned and left.
Without him there, my world got even smaller. There was nothing now. It was so quiet I couldn’t even hear myself breathing. My vision which was blurry to start with, got worse as the tears flooded my eyes. The isolation was the absolute worst thing I had ever experienced. I had nothing. I had no one to lean on, no information, and I realized I had no future.
I cannot explain what I was feeling. It wasn’t sadness; it was more so a sense of loss. It only lasted a few seconds, and then the anger hit me.
I was angry with his cavalier nature.
I was angry with the hospital.
I was angry with the neurology department.
I was angry at myself.
I was angry at myself for being sick.
I would walk out of a rehab facility six weeks later using a walker. I know I am fortunate, but it was challenging to maintain perspective when my world was collapsing around me.
The next 18 months consisted of immunosuppressant infusions, multiple relapses, and vision loss affecting both eyes. It was a constant cycle of vision loss and fighting for steroids to reduce the inflammation.
I spent hours trying to understand what was happening to me. I discussed the latest research and treatments with my care team because it seemed like we were missing something. It was exhausting and I was defeated.
Finally, my neurologist consulted an NMO specialist, Dr. Michael Levy. He requested I transition to new medication and I would travel to see him. In the months leading up to the appointment, the new medicine stabilized my vision and stopped the relapses.
At my appointment, testing confirmed I had MOG. The real tipping point was when he explained that the “five years” prognosis I had received was outdated and false. “You need to plan for a full life because NMO/MOG is not going to kill you.”

I began to realize I had been living in this shadow of a ticking clock. More accurately, my life had become so focused on the ticking of the clock. I wasn’t even living, just waiting for the end. I had been consumed by the loss of who I was and how this illness robbed me of my present and future. I realized a lot of my anger was rooted in the shame of having an invisible illness. I knew how colleagues and acquaintances saw me. I heard the whispers, “he doesn’t look sick,” when I missed work. “He doesn’t know what he is talking about,” as I tried to clear the brain fog that came with my medications. The murmurs from people as my voice cracked, and I stood there sweating during presentations because I was in so much pain and exhausted from just trying to keep my balance. I had bought into the stigma of chronic illness, doubting and devaluing myself.
It has been a challenging few years. I still feel defeated some days, but I know I have to keep fighting. I have to remember the lessons I have learned, so I don’t slip backward.
I learned that with NMO/MOG, there is no rhyme or reason. It is not your fault, so stop hating yourself.
I learned that the stigma of chronic and invisible illness is pervasive. We can not allow ourselves to get lost in the negativity, or we can be lost to feelings of worthlessness and shame.
I learned that we all have a voice, but we can amplify our power by building a team of advocates. Start by finding the person you trust most with your life and ask them to be your advocate; chances are you didn’t have to ask because they are already doing it. Start putting together the best team you can. Friends, family, doctors, specialists, build your community.
I have learned we must be active participants in our care. That means doing our homework and asking questions. It means understanding NMO/MOG are rare diseases, and many healthcare providers will not know what it is, so we must help educate them.
As a TSF Ambassador, I hope to encourage people to allow themselves some grace but understand we must constantly push forward because even the small victories are victories.
As a TSF Ambassador, I hope to help build the narrative of NMO/MOG based on the latest scientific data and around the examples of what patients have accomplished through perseverance and strength of spirit.
As a TSF Ambassador, I hope to help patients connect with opportunities that give them a better understanding of NMO/MOG, treatment options, and support systems.
As a TSF Ambassador, I hope to help develop resources and tools to educate medical professionals about NMO/MOG and help them understand their role in shaping patient perceptions and assisting patients in maintaining their dignity.
I hope you will join me in supporting The Sumaira Foundation as the organization continues to illuminate the darkness of NMO/MOG.